A few months ago, a story surfaced across social media — of Kamla Devi in Himachal Pradesh — crossing rivers on foot to vaccinate an infant. It stood as a powerful testament to the commitment of India’s frontline health workers. But if you look closely, beneath this inspiring image lies a more complex truth: in many parts of rural healthcare in India, access to even basic services continues to depend on extraordinary human effort rather than dependable systems.

This duality defines India’s healthcare journey.
On one hand, the country has made measurable progress. Through initiatives such as the National Health Mission (NHM), India has expanded its healthcare workforce by over 12 lakh between FY 2021–24 and administered more than 220 crore COVID-19 vaccine doses. Improvements in maternal and child health indicators, alongside programmes like Ayushman Bharat and the TB Mukt Bharat Abhiyan, signal a system steadily advancing towards wider coverage.

However, the immediate challenge still remains: ensuring these services effectively reach the most remote communities, while simultaneously strengthening state healthcare systems to sustain delivery and meet the targets of the Sustainable Development Goals (SDGs) and Universal Health Coverage (UHC).
Thus, within this context, it becomes pertinent to first examine what “accessible healthcare” truly means in India, particularly within the realities of rural healthcare in India.
The recent Health Parliament discussions brought forth a nuanced understanding of the multi-layered challenges spanning geography, infrastructure, workforce and trust that continue to shape access at the last mile.
Exploring the dimensions of accessibility in depth, this blog will also examine how corporate social responsibility (CSR) has evolved into a strategic enabler for taking quality healthcare to the last mile across India. Through sustained corporate partnerships with NGOs such as Smile Foundation, with over two decades of experience and more than 400 collaborations, growing efforts have been made to bridge the gap between policy intent and lived access.
Programmes like Smile on Wheels, Smile on Boat, Pink Smile, Swabhiman and physiotherapy initiatives for the trucker community exemplify how targeted, community-based interventions can translate systemic goals into tangible healthcare outcomes on the ground.

Accessible Healthcare: What does it mean in Rural India?
In policy discussions and boardroom conversations, the phrase “last-mile healthcare delivery” is frequently used to highlight the measure of India’s healthcare system’s success. However, this term demands special attention, when last mile healthcare delivery has to be done in the corners of rural India.
Should accessibility to healthcare be only limited to geographical limitations of the country? Should accessibility of healthcare services only mean the distance between a patient and the nearest health facility? Or does it extend to a more complex interplay of time, cost, awareness and the social confidence required to seek medical assistance.
These questions were brought into sharp focus during a recent Health Parliament dialogue organised by leading public health stakeholders, under the guidance of Rajendra Pratap Gupta, Founder of Health Parliament and senior sector experts, including Prof. (Dr.) Narendra Kumar Arora, Executive Director of INCLEN; Dr. Barnwal, Chief Executive Officer of National Health Authority of India; Professor K. Reddy, eminent public health expert; Mr. Mathew Cherian from CARE; Mr. Harish Iyer from the Bill & Melinda Gates Foundation; and Dr. Girish N. Rao, noted public health specialist.
Redefining Geographical Accessibility through CSR-Led Healthcare Delivery
At its most visible level, accessibility is about geography. India’s vast and diverse terrains – its mountains, forests and riverine belts create natural barriers that healthcare systems have to navigate through. As highlighted by Mr. Mathew Cherian, “the limited availability of quality healthcare within accessible distances” continues to define rural India”.
But what does “accessible distance” mean and how does it play a crucial role in India’s healthcare system?

Accessible distance cannot be only measured in kilometers between a village and a health facility. It is defined by the time taken, the terrain navigated, the cost incurred and the physical ability of the patience to make that journey. Mr. Cherian also highlighted that even today for many and especially the elderly of the vulnerable communities, a few kilometers journey to the nearest healthcare facility can be a significant disruption in their survival lifestyle.
Addressing these challenges, Dr. Rashmi Ardrey, Director Programmes Health of Smile Foundation highlights that “collaborative efforts must be invested in ensuring that accessibility is patient-centric”. She emphasised that quality healthcare in rural India must be designed as a continuum of care across the life-cycle – from antenatal and early childhood to adolescent, reproductive and elderly health.
Accessibility to healthcare must go beyond proximity, but about consistent, comprehensive and human centered services. In today’s time, Mobile Medical Units are playing a pivotal role in delivering curated care, screenings (eye, non-communicable diseases and cancer), anemia management, follow up care and referral support directly to the underserved communities.
“Mobile Medical Units (MMUs) challenge the idea that patients must travel to healthcare — healthcare must travel to them”. – Dr. Rashmi Ardey
Infrastructure Accessibility: India Needs Performance Driven Healthcare
India’s investments in healthcare infrastructure have been substantial, yet their effectiveness remains uneven. The persistence of understaffed and under-equipped facilities has given rise to what may be termed “passive infrastructure” systems that exist without delivering consistent value.
In light of the discussions at the Health Parliament, Ms. Sarita Pradhan, Head of Swabhiman, our intervention for women’s health and livelihood drew attention to a persistent and challenging gap in India’s rural healthcare system – the disconnect between infrastructure creation and actuarial service delivery.
“Health discussions are not effective if they do not yield results”. – Ms. Sarita Pradhan
Advocating for a strong public health leadership, structured monitoring and evaluation system, along with the use of real time data to guide decision making, Ms.Pradhan emphasises on collaborative efforts for making rural healthcare systems functional, accountable and continuously monitored to ensure real impact.
She also states that targeted interventions for adolescent girls, early childhood care and women’s reproductive health through data driven governance and collaborative efforts ensures females who are the minority groups within vulnerable communities access continuity of care at the community level.
By working within the community, she states that Swabhiman compliments the public system by combining awareness, on-ground engagement and service delivery- transforming passive infrastructure into active, accessible healthcare for marginalised women and their communities.
Human Resource Accessibility: Strengthening the Frontline
Healthcare delivery ultimately rests on human capacity. Accessibility, therefore, is not determined solely by infrastructure, but by the competence and responsiveness of those delivering care.
Today facilities may exist, but the shortage of trained healthcare professionals in remote areas continues to limit service delivery. Furthermore, this issue is not only numerical, but also one of retention in remote settings.
As Dr. Rashmi Ardey highlights, “strengthening frontline workers particularly in digital competencies is critical in an evolving healthcare ecosystem”. She also states that face to face interactions with medical professionals satisfies a crucial element that helps in building trust – the “touch and feel” care; especially important for the elderly populations, who are still not well versed with digital tools.
Furthermore, Mr. Harish Iyer’s observations at the Health Parliament further deepened the conversation around human resource readiness in a digitised healthcare ecosystem. He underscored that the integration of digital health tools can only be effective when frontline workers are adequately trained — not just in operating technology, but in interpreting and applying it within real-world community settings.
He also highlighted that disease surveillance systems, increasingly driven by digital platforms, still rely heavily on human intervention for accurate data collection, validation and response. Without skilled personnel on the ground, even the most advanced systems risk becoming underutilised.
Thus, strengthening frontline capacity is not optional — it is foundational and its future must not be solely a public system’s responsibility, but collaborative efforts must be invested in building a workforce that can seamlessly integrate technology with human judgement, ensuring both efficient service delivery and responsive public health systems.
Economic Accessibility: From Coverage to Comprehension
While infrastructure and workforce challenges often dominate the discourse, the economic condition of individuals remains one of the most decisive barriers to healthcare access in rural healthcare in India. For many households, seeking medical care is not just a health decision, it is a financial calculation.
Loss of daily wages, cost of travel, diagnostic expenses and medication collectively discourage timely care seeking. As a result, illnesses are often delayed, under treated or ignored until they become critical. A loop where poverty and poor health get intertwined with each other.
Thus, addressing this grave challenge, the discussions at the Health Parliament brought forward the importance of strengthening financial protection mechanisms, particularly through Universal Health Coverage – a foundational requirement for equitable and inclusive growth of the nation.
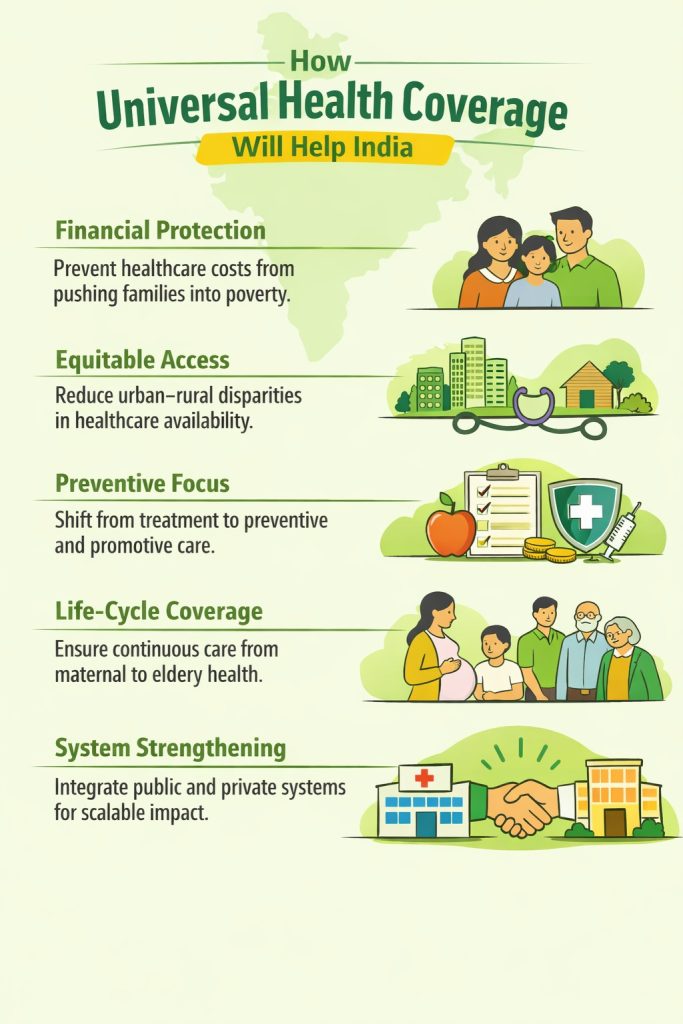
To ensure healthcare is more accessible, Professor K. Reddy, eminent public health expert stated that “Universal Health Coverage should offer both service coverage and financial protection” – this dual focus will ensure that affordability and availability will go hand in hand”
Reinforcing this Dr. Ardey, Smile Foundation states that “Universal Health Coverage which includes preventive and promotive care is the only way forward”. UHC coverage must move beyond financial coverage to a more holistic life cycle approach to healthcare.
At the implementation level, Dr. Barnwal, Chief Executive Officer, National Health Authority of India noted that “health coverage in India has reached approximately 65% of socially vulnerable populations,” signalling progress, yet also indicating the remaining gap in universal inclusion while, Ms. Pradhan pointed out that “reducing out-of-pocket expenses is important for expanding service coverage,” but financial protection alone is insufficient without effective execution and awareness.
And this is where CSR partnerships with NGOs in India like Smile Foundation can help in bridging an essential gap in India’s rural healthcare, by not just being a supportive functionary, but a critical bridge between policy intent and on ground execution. Highlighted by Mr. Satnam Singh, Senior General Manager of Health at Smile Foundation, he states that CSR partnerships with credible NGO partners can create measurable impact.

Socio-cultural Accessibility: The Role of Trust in Healthcare Utilisation
One of the most overlooked issues of accessibility to quality healthcare in rural India is the social cultural factors. The presence of healthcare services does not automatically translate into their utilisation, as a critical barrier lies in trust. Rural communities tend to prefer familiar and relationship driven interactions over impersonal or purely digital interfaces.
This perspective was reinforced by Dr. Gupta’s analysis of health determinants, where he showed how only 10–20% of health outcomes are influenced by clinical care, while a significant proportion is shaped by environmental factors (24%), food systems (20%), genetics (20%) and individual behaviour (10–15%).
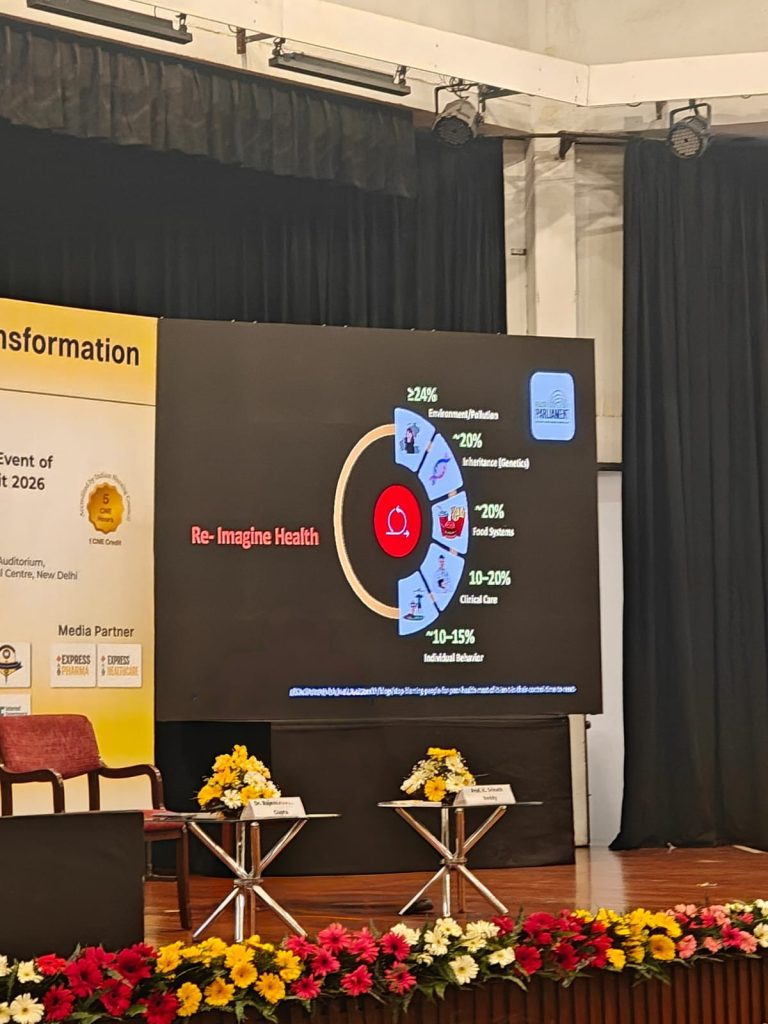
Weak community engagement further limits acceptance of healthcare systems, creating a gap between availability and actual usage. In this context, accessibility extends beyond physical reach — it becomes psychological and relational. Without trust, even well-designed interventions risk remaining underutilised.
Therefore, the only way forward is to ensure that healthcare does not operate in isolation or just as a responsibility of the public healthcare system. Building trust, influencing behaviour and engaging communities are central to improving outcomes, making socio-cultural accessibility a critical lever in achieving meaningful healthcare access.
Partner with Us: Deliver Healthcare that Reaches
Achieving accessible healthcare within rural healthcare infrastructure and system in India, requires a system-level shit–from integrating geography, infrastructure, workforce readiness, affordability and trust into a cohesive delivery model.
As the Health Parliament discussions highlighted, that access is not a single variable but a factor which shapes the continuity of the real world conditions. And this is exactly, where CSR partnerships with Smile Foundation can move beyond compliance to strategic interventions for building affordable, accessible and equitable last-mile healthcare delivery mechanisms while also strengthening the implementation ecosystem and generating measurable and sustainable social impact – ensuring that no life suffers because of inadequate or untimely care.
Sources:
Brave Nurse Crosses Flooded Stream In Himachal Pradesh To Vaccinate Baby